HOW TO MANAGE/TREATACHILLES TENDINOPATHY WITH 3 EASY PHASES/STEPS?
Achilles tendinopathy is a common overuse injury that occurs as a result of repetitive strain on the tendon. This article will demonstrate the mechanisms involved, common symptoms and what to look out for, risk factors but most importantly how you can treat this pain at home. Here at physiophi, our aim is to educate the patient to allow you to manage your pain. If however you still need more guidance we have physiotherapy clinics located in Jindalee and Darra who will accelerate your recovery.
WHAT IS ACHLLES TENDONOPATHY?
Accumulation of compressive forces on the tendon can lead to an abrupt injury of the complex. Over time this can cause further degradation of the tendon complex and ultimately lead to a rupture of the Achilles tendon.
THE MECHANICS INVOLVED
The Achilles tendon is the strongest tendon in our bodies, meaning it manages the highest tensile loads. It originates from both the gastrocnemius and soleus muscles (the upper and lower portions of the calf muscle) and attaches into the bottom of the calcaneus, otherwise known as the heel. Repetitive loading with excessive compression can cause microtears, inflammation of the tendon sheath and degeneration or in a worst case, a rupture of the Achilles tendon.
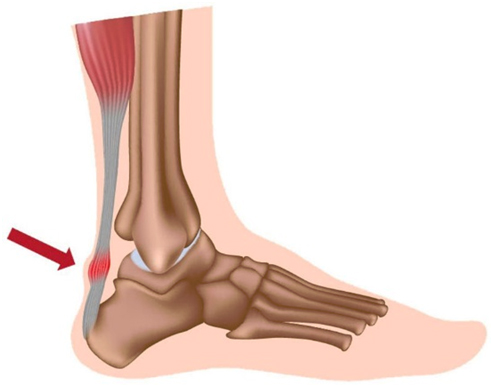

Credit: https://inertiahealthgroup.com.au/achilles-tendinopathy/
COMMON SYMPTOMS AND WHAT TO LOOK OUT FOR
Common symptoms for Achilles tendinopathy include:
- Morning pain: This is a primary symptom of Achilles tendinopathy due to the Achilles complex requiring full ranging in order to walk after waking. Stiffness is typically observed after nocturnal immobility. As a result, symptoms are typically felt in the local and immediately adjacent regions.
- Swelling and pain: These symptoms can be present but are less common.
- Sensitivity: Sensitive regions can manifest along the Achilles tendon.
- Pain on walking
RISK FACTORS
These are the following risk factors for Achilles tendinopathy. The list is extensive but not exhaustive. There is more research that highlights new risk factors such as prior lower limb injuries and alcohol use as risk factors.
- Runners in the 30-60 year age range
- Increased pronation of the foot
- Obesity
- High blood pressure
- Rapid changes to load
- Chronic diseases that affect tendon health (diabetes, rheumatoid arthritis or hypercholesterolaemia)
- Prolonged steroid use
- Family history of tendinopathy
- Prior lower limb injuries (eg. tendinopathy or fractures)
- Alcohol consumption (greater than moderate)
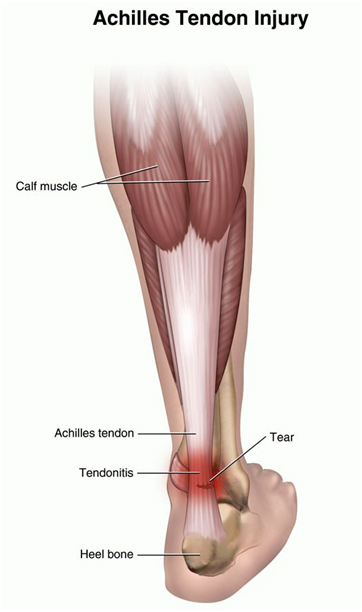
Credit: http://www.completesportscare.com.au/2015/04/top-4-treatments-achilles-tendinopathy/
WHAT CAN I DO TO MANAGE MY INJURY AT HOME?Achilles tendinopathy is not a condition that handles total rest well and patients should continue with recreational activities within pain tolerance while participating in rehabilitation. This overarching concept serves as the cornerstone for early intervention and management.
DOs:
The concept of RICE (Rest, Ice, Compression and Elevation) can be applied:
- Icing post-activity or when pain flares up
- Compression wraps can help reduce movement of the tendon
- Elevation of the leg can ease swelling if present
- Most important relative rest is primarily the key to avoiding further exacerbation of symptoms.
- Exercise therapy is the most important for long-term healing and overall recovery. This aspect would focus on appropriate loading of the tendon alongside the subsequent aim of gradual return to activity, be it sport or daily function. There are three phases of loading of the Achilles tendon:
- Phase 1: Isometric loading of the Achilles tendon involves doing a heel raise on one leg and maintaining. If symptoms are highly irritable, it is recommended to do double leg holds and for a shorter duration.

- Phase 3: Plyometric loading is the final stage and extremely important to the longevity of the Achilles tendon and reduction of future recurrences. This is done through hopping exercises that retrain the Achilles' capacity to absorb and release energy. Ultimately this phase ties into return to sport and normal daily function.
DON'Ts
Reducing or stopping the triggering activities is paramount.
- No uphill or downhill walking or running
- If explosive activities such as sprinting, jumping and rapid changes of direction aggravates symptoms, stop those activities
- Do not ignore the symptoms
- Excessive stretching of the tendon will cause further compression of the tendon
If at-home solutions do not help to reduce pain, we at Physiophiexcel at accelerating your recovery to have you pain free and moving freely. There are a myriad of solutions to treating Achilles tendinopathy that can aid in faster and more effective recovery.
- Optimizing biomechanics of gait and posture
- Controlled tendon loading exercises
- Adjunct therapy through the use of Extracorpeal Shockwave Therapy can assist to reduce the pain and breakdown chronic scar tissue.
- Taping can be done to reduce further stress on the Achilles tendon.
- Dry needling of the Achilles and surrounding tissues can serve to reduce pain and irritation of the area.
- Massaging the calf can reduce passive and active tensile forces into the Achilles and therefore aid recovery.
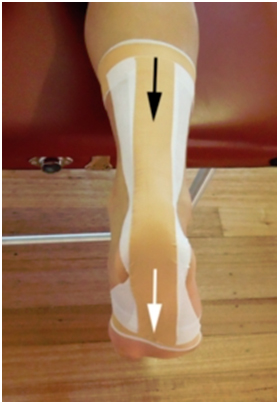
Credit: https://www.physioadvisor.com.au/health/taping-techniques-lower-body/achilles-tendon/
PLEASE CONTACT US ON: (07) 3172 4332 TO HAVE A CHAT WITH OUR FRIENDLY STAFF OR SIMPLY BOOK ONLINE ON: WWW.PHYSIOPHI.COM.AU
REFERENCE LIST
Knapik, J. J., & Pope, R. (2020). Achilles Tendinopathy: Pathophysiology, Epidemiology, Diagnosis, Treatment, Prevention, and Screening. J Spec Oper Med, 20(1), 125-140.
Ogbonmwan, I., Kilcourse, E., & Gupta, S. (2020). Achilles tendinopathy: a guide for general practice. Br J Gen Pract, 70(700), 563-564. https://doi.org/10.3399/bjgp20X713381
Touzell, A. (2020). The Achilles tendon: Management of acute and chronic conditions. Aust J Gen Pract, 49(11), 715-719. https://doi.org/10.31128/AJGP-07-20-5506
van der Vlist, A. C., Breda, S. J., Oei, E. H. G., Verhaar, J. A. N., & de Vos, R. J. (2019). Clinical risk factors for Achilles tendinopathy: a systematic review. Br J Sports Med, 53(21), 1352-1361. https://doi.org/10.1136/bjsports-2018-099991
